 The latest study from researchers at CaHRU was published this month (July 2017) in BMC Medical Infromatics and Decision Making. Entitled ‘Perceptions on use of home telemonitoring in patients with long term conditions – concordance with the Health Information Technology Acceptance Model: a qualitative collective case study‘, and co-authored by Dr Jo Middlemass (visiting fellow), Jolien Vos (doctoral student) and Prof Niro Siriwardena (director), the study formed part of the process evaluation of a large multicentre, multinational trial funded through the European Framework 7 programme, Clinical tRials fOr elderly patients with MultiplE Disease (CHROMED: clinicalTrials.gov Identifier: NCT01960907).
The latest study from researchers at CaHRU was published this month (July 2017) in BMC Medical Infromatics and Decision Making. Entitled ‘Perceptions on use of home telemonitoring in patients with long term conditions – concordance with the Health Information Technology Acceptance Model: a qualitative collective case study‘, and co-authored by Dr Jo Middlemass (visiting fellow), Jolien Vos (doctoral student) and Prof Niro Siriwardena (director), the study formed part of the process evaluation of a large multicentre, multinational trial funded through the European Framework 7 programme, Clinical tRials fOr elderly patients with MultiplE Disease (CHROMED: clinicalTrials.gov Identifier: NCT01960907).
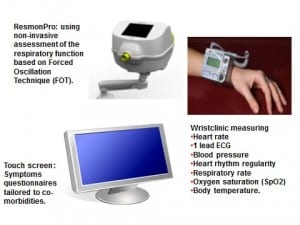 This was a qualitative interview study of patients aged between 60 years and over together with their partners or relatives where applicable on implementation of a telemonitoring system in their homes for chronic obstructive pulmonary disease (COPD) combined with heart disease. Patients and their relatives were largely positive about telemonitoring but they expressed concerns regarding health professional access and attachment; heightened illness anxiety and desire to avoid continuation of the ‘sick-role’; the need for good organisational processes and informal support. Ease of use was connected to equipment design being suitable for older people. Participants felt it was important to establish trends in health status, to enable detection of early signs of infection and increase the potential for patients to self-manage.
This was a qualitative interview study of patients aged between 60 years and over together with their partners or relatives where applicable on implementation of a telemonitoring system in their homes for chronic obstructive pulmonary disease (COPD) combined with heart disease. Patients and their relatives were largely positive about telemonitoring but they expressed concerns regarding health professional access and attachment; heightened illness anxiety and desire to avoid continuation of the ‘sick-role’; the need for good organisational processes and informal support. Ease of use was connected to equipment design being suitable for older people. Participants felt it was important to establish trends in health status, to enable detection of early signs of infection and increase the potential for patients to self-manage.
 The main trial results have been previously presented at the European Respiratory Society conference and these are currently being prepared for publication. The overall conclusion of this sub-study was that to increase home telemonitoring acceptance among older people, consideration of equipment design and organisational factors was important.
The main trial results have been previously presented at the European Respiratory Society conference and these are currently being prepared for publication. The overall conclusion of this sub-study was that to increase home telemonitoring acceptance among older people, consideration of equipment design and organisational factors was important.
By Niro Siriwardena














